Building capabilities for customer centric decision-making using time to value
In our latest blog post relating to Intelligent CX, Curzon Analyst Milla Bradstock explores how to build capabilities for customer centric decision-making using Time to Value.
Time to Value, as a metric, initially rose to fame among software companies and its insights now drive improvements in a range of business contexts. In a customer context, it is described as the length of time between a customer purchasing a product or service and seeing the value of that action. Yet to untap the metric’s full potential, businesses must take a longer-term view of its application that goes beyond resolving customers’ immediate needs.
As T2V requires organisations to understand the value of their product or service from a customer’s perspective, it entrenches customer-centricity into the way businesses think about their services. At a time of rapidly shifting customer priorities, organisations that take this approach will be well placed to remain aligned to the needs of their customers.
Measuring Time to Customer Value
Tracking T2V builds a picture of your present customer journey, which will inform solutions to better fulfil customer needs. However, you can only track T2V if you know what ‘value’ is in the eyes of your customer. The definition of value will, of course, differ amongst your customers, but we can start to break down this metric into two sub metrics:
-
Time to Basic Value – The time it takes for a customer to see the minimum amount of value from your product or service. Delivering on this metric doesn’t lead to customer loyalty necessarily, but will increase conversion.
-
Time to Exceeded Value – The time it takes for a customer to see enough value to exceed their expectations over a longer period of time. Delivering on this metric reduces churn, builds loyalty and increases customer lifetime value.
For example: A travel app with an easy to use interface and intuitive search results will deliver on the Time to Basic Value metric. However, its Exceeded Value will be realised only when it helps a customer have a good holiday i.e. booking a place to stay using the platform.
T2V helps businesses identify obstacles to customer satisfaction, which inform solutions for long-term value creation in the eyes of their customer. For SaaS businesses, onboarding is essential to their customers seeing value from their purchase, which creates the challenge of motivating customers to complete the process.
Focusing on accelerating T2V at this point in the customer journey can therefore decrease customer churn and improve satisfaction. Automated onboarding can be an effective tool, delivering frictionless setup and easy deployment through product tours, in-app messages and onboarding checklists. In tune with customer demands for instant service and ultimate convenience, this tool enables customers to seamlessly see the value of their purchase for themselves.
Implications for organisations
- Move the narrative from Customer Needs to Customer Value
- Focus on Customer Engagement beyond the initial purchase
- Measure and monitor customer engagement throughout the Customer Lifecycle
- And, of course, ensure the engagement delights the customer every time
How we can help
T2V is just one of the tools that we employ to help our clients improve customer value. Businesses that invest now in strengthening their capabilities for meaningful customer engagement will build the resilience necessary for long-term success.
Get in touch to explore how we can help your organisation create lasting value for your customers.

Rachna Trehan leads Curzon Consulting’s Intelligent CX practice. Connect with Rachna on LinkedIn or contact her to discuss how this could apply to your organisation.
Other members of the Intelligent CX team
CONTACT US TO FIND OUT HOW WE CAN HELP
Future of work: healthcare med reps transformation
In his latest blog post relating to Future of Work, Curzon’s Managing Consultant Rodrigo Quezada Dighero focuses on the transformation of healthcare medical sales reps.
Exploring how the pandemic has disrupted the face-to-face salesforce, and the unique opportunity this presents to adapt the operating model for future success.
The effectiveness of a disrupted salesforce
One year into the pandemic and face-to-face sales look very different from 12 months ago. Medical Reps are facing exceptional challenges in reaching their sales targets, as restrictions on in-person meetings with HCPs continue.
The gravity of the situation is reflected in the 16 new drugs launched during COVID-19 lockdowns, that are at risk of sales failures, according to one pharma consulting group.
However, the lifting of lockdowns is unlikely to return the industry back to ‘normal’. In fact, the evidence shows a stark reality for in-person sales.
-
About 60% of surgeons believe that restrictions on in-person sales are likely to remain even after a Covid-19 vaccine is available and lockdown restrictions abate.
Percentage who believe restrictions on face-to-face visits are likely to continue after Covid-19
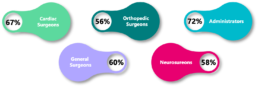
Moreover, the changing landscape is not just a result of the pandemic; it’s expedited the necessary changes, but fundamentally, companies have been very slow to adapt their operating models to address the needs and wants of their customers and workforce.
-
Of the 75% of physicians who preferred in-person visits from Medtech representatives prior to Covid-19, 47% would now opt for a virtual exchange or less-frequent visits.
-
Many physicians once sceptical of any virtual interaction with sales reps now report these exchanges are high quality and offer a much better experience.
Healthcare providers are demanding more from pharma, as they seek greater value from their interactions with Med Reps.
-
69% of doctors now want digital patient education
-
67% want more education on remote patient care
-
65% need specific information on conditions relative to COVID-19
-
65% require information to help patients access labs, tests and imaging
It’s clear as medical professionals endure the uncertainty caused by COVID-19, changes are here to stay, and adaptation is crucial to success.
Identifying the opportunity - a new way of working
Digitalisation has accelerated the Next Normal requiring pharma operating models to adapt, or in some cases, completely transform to help them to thrive or even survive.
In this context, the need to provide refined, enriched collateral to healthcare providers and doctors demands an evolution from face-to-face meetings and conferences into a hybrid exchange of virtual and in-person meetings, steered by medical reps.
Percentages of doctors who prefer in-person sales visits
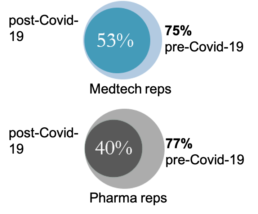
However, in order for this to be fully realised, pharma companies need to adjust and develop their salesforce capabilities. In another study, research shows that only 26% of pharma reps get coaching personalised to their needs. A focus on sales coaching, through integrated, personalised and value-driven interactions will support med reps to identify target prospects and align the products to the needs of the HPC, through their preferred communication channel.
Moreover, managers and leaders need to align sales & marketing, to ensure a collaborative approach to fully understand the customers and the local market they operate in. Communication and insight must flow both ways to drive communication strategies, content creation and support product development.
Our approach
Our approach to New Ways of Working accelerates the adaptation to the digital business model, focusing on the delivery of required capabilities and the evolution towards a hybrid model.
For this specific transformation, we focus on four of the five key areas
-
Organisation
-
Collaboration and Hybrid Solutions
-
Smartworking Processes
-
People & Leadership
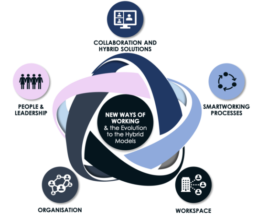
Organisation
- Develop strategies that assist medical reps throughout the sales process, tailored to every customer touchpoint.
- Establish hybrid teams that can develop relevant, channel-specific, timely content to empower the med reps.
- Foster internal engagement and alignment by creating a purpose-based organisation with a relentless focus on value-add customer service.
- Entrench company culture to sustain new ways of working and improve business agility – always listening… constantly evolving.
Collaboration & Hybrid Solutions
The virtual nature of teams and work communities spearheads the need to adopt solutions that enhance and facilitate effective remote interactions.
- Optimise team relationships, roles & interactions to enhance hybrid ways of working.
- Design and implement collaboration solutions applied to the business and team leadership.
- Adopt collaborative tools, enabling sales & marketing teams to share opportunities that improve the quality of exchanges, content creation and value-based interactions regardless of location.
Smartworking Processes
Achieving process transformation through re-engineering & automation to create a generation of agile, flexible, efficient and collaborative working dynamics.
- Redesign smartworking processes, harnessing automation and flexibility to accelerate change and bring the hybrid model alive.
- Employ digital tools to evolve sales, HCP engagement and bring the customer experience to the forefront of every interaction.
- Remove silos to cultivate employee engagement and shared knowledge/opportunities.
People & Leadership
Evolution of culture and people is the foundation of Digital Transformation enabling leaders of pharma companies to steer a change in behaviour and actions.
- Adapt the hybrid model and embed culture based on learning and sharing.
- Develop salesforce capabilities with a focus on digital skills, converging efforts to support sales requirements through content creation and content sharing.
- Embed a coaching culture that fosters learning and sharing.
- Deploy cultural change that embraces and cements the New Normal.
The time to act is now
We work with pharma businesses to deliver New Ways of Working that accelerate the adaptation to the digital business model. Ultimately our work helps businesses to grow, improve customer retention and discover new opportunities.
Ask us how we can help your organisation to transition into the New Ways of Working putting your salesforce ahead of the curve.
CONTACT US TO FIND OUT HOW WE CAN HELP
Future of Work insights
Creating a strong operating model in the digital age
In our latest blog post relating to Intelligent CX, Curzon Associate Partner Rachna Trehan explores how to start creating a strong operating model in the digital age.
It is undeniable that we are deep in the ‘digital age’, or even the ‘post-digital age’. Different organisations are still at different levels of digital maturity and have shown a remarkable capability to change.
I think we can also agree that “Customer Needs” have changed. Browsing, selecting, influencing, engaging, buying, renewing… these all have new meanings which organisations are responding (some leading the way) to keep up with.
So, let’s take this argument further. How do we ensure organisations are set up to adapt to change rather than react to it? Whether it’s technology advances, changing customer needs or business continuity, they need to be agile and flexible.
The answers lie in transforming your operating models.
Four pointers to help you start to create a strong operating model in the digital age
Here are four pointers that we recommend in the sales and service space:
Build Agile Delivery Cells
- Create Change cells around customer journeys that move fast, drive change, engage different talents and build an AGILE mindset.
- Build flexible organisational structures enabling the growth and deployment of change cells.
- Focus on outcomes, not outputs, in every part of the organisation. Change your metrics, incentives, and culture to be customer outcomes focussed.
- Build processes / journeys with Systems and Design Thinking but with an agile mindset.
- Collaborate with customers… before finalising products, journeys, metrics, operating models.
Focus on building platforms, not just software solutions
- Build or transition to cloud-based platforms and collaborative solutions.
- Ensure service designs are accurately reflected through the systems, and deliver the desired outcome.
- Think end-to-end connectivity across customer journeys and potentially across the value chain.
Keep your employees happy
- Happy employees are motivated to work with agility, create happier customers and generate more revenue.
- Employee Happiness is actually a measure – there are ways to make it tangible, and track impact on the top/bottom line.
- Invest in your people – Train them to “add value” to the customers / company. Having high quality human conversations can actually be a differentiator.
- Flexibility in resourcing and ways of working – “physical boundaries” and “typical employee profiles” are a thing of the past. The world is your oyster. AI powered WFM solutions can take the pain away.
Focus on Customer Engagement
- Get customers to engage with your products, journeys and people.
- Learn from these engagements and improve the happiness quotient around them.
- Spread the word within your organisation – Sales, Loyalty, Up/Cross Sales all depend on customer engagement.
Get in touch
These four areas will help you start your journey towards creating a strong operating model in the digital age.
Curzon provides the experience to prepare our clients for the future and deliver tangible results. See you on this exciting journey.

Rachna Trehan leads Curzon Consulting’s Intelligent CX practice. Connect with Rachna on LinkedIn or contact her to discuss how this could apply to your organisation.
Other members of the Intelligent CX team
CONTACT US TO FIND OUT HOW WE CAN HELP
Future of work: navigating uncertainty through agility
In his latest blog post relating to Future of Work, Curzon Managing Consultant Rodrigo Quezada Dighero in collaboration with Silviu Paraoan, explores how an agile approach focused on people and customers can lead to competitive advantage. This is particularly important now, as businesses are navigating uncertainty caused by COVID-19.
How employee and customer centricity are the key to an agile organisation
In Q4 2019, companies were finalising growth targets, key priorities, strategy, hiring needs and budget. Yet many businesses have spent 2020 in survival mode, putting the 3 year strategy on hold to necessitate a short term focus on business continuity.
Now, as many businesses enter Q4 2020, leaders revisit the original 3-year strategy plans as they look towards recovery. This inflection point is a great opportunity to adapt to the new world order and practice strategic foresight, as J. Peter Scoblic would say. In fact, this is not just an opportunity; the reality demands that you revisit strategy, adapt, and align your capital expenditure to this new paradigm. Becoming agile is the name of the game, to remain in the game, and to stay ahead of the rest of the players amid the disruption. In this new reality Winner takes All, and to be one, you need, you really need to reassess, adjust and plan your strategy.
Business continuity is one way of responding to disruption. But many people – including me – hold the belief that business continuity won’t be enough. Furthermore, it could put you behind competitors and faced with the risk of becoming obsolete. The time is now to think holistically about how to create opportunities in this new reality and adjust your business and operating models to serve the current and future needs of customers and employees. Two key areas are:
The agile organisation – how are you going to create an organisation that is adaptable, flexible and agile? When I talk about agile, I don’t mean a system. I’m referring to an agile organisation mindset characterised by collaboration and creativity. This means setting up the supply chain, procurement, and people strategies. It means employee engagement and training to encourage creativity and innovation from sales and marketing to operations and supply chain. It means developing a strategy to strive and thrive.
Customer centricity – how are you going to deliver products and services? Businesses will need to evolve to serve in this new environment in which customers have different expectations and needs.
The agile organisation
As you conduct your strategic thinking on this first area, there are a few key concepts to bear in mind:
- Overcommunication is key – align employees behind strategic priorities through clear and empathetic communication
- Use technology to augment, not replace, people
- Focus on people instead of processes
- Be flexible
- Collaborate – look for cross-functional collaboration. Maybe it’s time to start building that Business Ecosystem we have been theorising about for so long and make this opportunity a long term approach
- Keep it simple – this is not a time for dense multi-page documents. The agile approach of single-page, action-oriented documents with crystal clear communications is the order of the day.
- Embrace the new cultural and behavioural shifts
Customer experience
How will companies and their operations evolve to recreate the customer experience? Changes will of course create both challenges and opportunities in technology and creative approaches to developing new ways of delivering new systems and products. Done well, this can create significant competitive advantage.
The reimagining of customer experience is a challenge shared across industries. For example, how is banking going to change to better serve its customers? What will supermarkets do to enhance the shopping experience in this new environment?
According to an article in the Harvard Business Review, Bank of America converted more than 3,000 employee roles to meet the demand of additional customer calls during the crisis. In China, companies began an employee “sharing” program across the grocery store industry to meet the need for the delivery of grocery store items.
Agility is key to navigating uncertainty and understanding, meeting and exceeding new, evolving and emerging customer expectations.
Recalibrating strategy
The process is not about recreating or redesigning your strategy. It’s about realigning and calibrating what you had to serve in this new environment. What is the gap that has been created between your previous strategy and this new normal, and how are you going to serve your customers?
From my experience, you can do it from four dimensions:
- Digital – What technology is yet to be discovered or that is in place today that can help you to bridge that gap?
- Systems and processes – consider what current systems and processes will need to be replaced, modified, or switched to allow a better level of flexibility? What can be changed to allow employees to perform their job functions with excellence?
- Capabilities – how are you going to develop the required capabilities into your people for them to identify those gaps and cover them through the digital dimension or processes and systems?
- Physical location – covers the physical location. It is common to hear industry leaders talk about a spike in satellite offices. Is that the right option for you? Do you need to rethink your footprint or can you take advantage of your current location and layout to benefit new operations?
Finally, the most critical part of transformation is collaboration. By listening to employees and customers, you can strategise, realign the operations, and quickly redeploy the strategy in an agile way within the new normal environment.
A few companies are taking actions into this direction, and results are actually promising. One clear example is Nike which beat profit estimates in the quarter ending August 31st 2020. With physical sales decreasing due to COVID-19, Nike shifted focus to direct sales to consumer and digital channels. Their adjustments in strategy led to 82% increase in digital sales.
Key questions for leaders
- How will you quickly adjust your business strategy and associated goals to reflect the turbulence in the marketplace and maintain a competitive advantage?
- Is your workforce engaged, productive, and healthy during the continued disruption?
- Is your business learning and adapting to be prepared for the next disruptor?
- How has your service or offer changed because of COVID? (Front office and back office)
- How has overall the customer experience changed in your business/sector due to COVID?
- How have you been adapting your operations over the last 6 months and how are they going to keep evolving based on needs?
These questions should help you to identify areas of focus and strategic priorities that your people can work towards.
The time to act is now
We work with businesses to deliver an agile framework to determine the key factors to quickly adapt, optimise people strategy and enhance your digital capabilities. Ultimately our work helps businesses to grow, improve customer retention and discover new opportunities.
CONTACT US TO FIND OUT HOW WE CAN HELP
Future of Work insights
Understanding the new workforce drivers
Curzon Managing Consultant Rodrigo Quezada Dighero shares his thoughts on the new workforce drivers.
Covid-19 is disrupting the ways in companies can engage and reward their workforce, traditionally a key factor to retain talent. Organisations should be using this opportunity to re-evaluate reward programmes and incentive models, paying close attention to employees’ changing values.
A time of disruption
Before the coronavirus pandemic, companies employed a wide range of benefits to engage and reward their employees. These spanned from pay increases and bonuses (monetary incentives), to office experiences such as in-house chefs, ping pong tables and lounges. Creating a great experience in the office was key to having a competitive edge with your rewards system.
Up until the pandemic, it could be said that key employee engagement drivers included the above listed rewards. However, the lockdown, enabling many to work from home, created a shift. A recent study showed that economic disruption and uncertainty brought high levels of anxiety for employees over their personal job security for over 64% of the global workforce. The result has been people committing long hours and working harder. For example, Rightmove Chief executive Peter Brooks-Johnson, said in March: “I’ve been encouraged by how seamlessly people have adapted to working from home and how productivity has increased over the past few months.” The property website has over 530 staff who moved to home-based working since March.
The new driver for employees shifted from an enjoyable working environment to keeping their jobs and their financial stability. For many, this was also balancing household responsibilities, taking care of family and working in cramped conditions. Suddenly work/life balance became a work/life blur. People adapted in order to maintain business continuity, but at a cost. Furthermore, a recent study showed that 62% of people trusted their employer to respond responsibly to COVID-19.
Now, as companies look to the horizon, people are also considering what the new normal will be for them in their working lives. Companies need to be aware of this when planning workforce engagement principles for the future. The focus is no longer on solving employees problems within the office, but rather it should include their household and life challenges.
It is important for companies to understand what the new drivers for employee engagement are, and adapt to better serve those new drivers. This will provide the right incentive for employees to remain engaged, creating a new environment to not just survive but thrive at work.
A great start
In May, Twitter communicated that staff would be able to work remotely forever if they desired. The communication from Jack Dorsey is an example of paying attention to what people were struggling with, a new reality. This was strengthened by an additional benefit – the provision of equipment to transform their home into an office.
The pandemic has increased the trend of employers playing an expanded role in their employees’ financial, physical and mental well-being. Support has included enhanced sick leave, financial assistance, adjusted hours of operation and child care provisions, special allowances for work-related need such as Ergonomic chairs, monitors and Wi-Fi. In the case of a workforce that cannot operate remotely, setting extra precautionary measures such as safe commuting alternatives and workplace adaptation have been the norm.
The current economic crisis has also pushed the bounds of how employers view the employee experience. Personal factors take on a new importance for organisations and employees alike. Employing a range of measures can be an effective way to promote physical health and improve the emotional well-being of employees.
But there’s still no clarity on the long term impact of COVID on the workforce.
The time to act is now
It is often difficult to create change or transformation within organisations. The present time offers an opportunity for organisations to change their people strategy and create more efficient and productive ways of working. Key considerations are:
Design from your people, not for them
Ask your workforce, and put yourself in their shoes, this is an extremely important time to listen to what your workforce cares about the most, and design your plans and drivers around it.
Communicate often with authenticity, compassion and confidence
One of the actions we saw in our clients that provided calm to high levels of anxiety on their workforce was continuous, honest and open communication.
Proactively seek feedback from employees and give them a voice, and let them lead. Ensure leaders share their own COVID-19 experiences.
Build trust with people through purpose
Uniting employees under a common purpose can be a strong motivating factor which is important during a challenging journey of change. Purpose-driven organisations are more flexible and better at navigating uncertainty.
Support households, not just employees
Workplaces may be starting to reopen, but uncertainty prevails for employees in other areas of life.
This highlights the importance of mental health support, employee assistance programmes and well-being initiatives to help people adapt during a difficult time.
Revisit policies, focusing on the most vulnerable groups, such as temporary workers, people with disabilities, single parents or those who lack adequate health benefits.
Remember, design the plan by asking your people; prepare your people to be in action, engage them into the new order, and finally, prepare to lead. Times like these require active leadership and consistent communication.
Working from home or living at work?
COVID-19 has brought unprecedented challenges. Many companies have risen to the occasion, acting swiftly to safeguard employees and migrate to a new way of working that most business-continuity plans hadn’t envisioned. Across industries, leaders will use the lessons from this time to re-imagine how work is done, and what role offices should play, in creative and bold ways.
This pandemic has also highlighted that work and personal life are closer than once thought. Merging work and home over the past months proved that there are new motivators that people are looking for from organisations. Understanding this new reality is crucial for companies to recruit and maintain talent, so adapting quickly is key.
The time to act is now. This is a unique opportunity to engage your people, address change and understand what the new reality demands from your business.
For that, you will need to listen and adapt. We have experience in change and we have put some approaches to help you in that process. We can help to design and implement a strategy that helps your organisation to manage change and drive workforce effectiveness, efficiency and engagement.
CONTACT US TO FIND OUT HOW WE CAN HELP
Future of Work insights
The future of work
The Future of Work
COVID-19 has accelerated and amplified Future of Work trends impacting HR organisations and their enterprise partners.
As businesses work towards recovery and return to work, we explore what an effective people strategy and change management looks like.
Many organisations are now in a reactive mode and focused solely on business continuity. We can help organisations adapt their strategy and return to key fundamentals or create a new path forward.
Get strategy back on track – or a create new path. We will guide your strategy adaptation and a clear plan for execution.
Organisations are set to transform their workforce and workplace. It is increasingly important to be more agile while re-imagining the employee experience and emerging technologies to be successful in times of rapid change.
Organisations must align around a vision of future-ready talent and new modes of working. This means embracing the world of human, machine, physical, and digital to make near-term progress that delivers long-term opportunity.
Now is the time to develop and execute a human-centric plan for peak workforce efficiency and effectiveness.
As businesses begin their return to the workplace, there are a lot of questions to consider. Keeping people at the forefront of every decision is critical to a successful return. Our contact tracing solution, together with Nextconinent citizen Umlaut, helps organisations to keep their employees safe.
In collaboration with Point B
We have collaborated with our global consulting alliance (Nextcontinent) partners, Point B, to provide cross-border expertise on the future of work.
Some of their workforce experience insights:
- Guiding principles of remote working
- Inclusion in a virtual workspace
- Business continuity while working remotely
- The future of work is now webinar
Read our latest thinking below.
Future of Work insights
CONTACT US TO FIND OUT HOW WE CAN HELP
Re-assessing cost after COVID-19
The global COVID-19 pandemic has provoked the need for businesses to re-assess their footprint and cost base across the supply chain. John Mason, Manufacturing & Engineering Services Partner at Curzon Consulting, considers the case for structural change.
Re-assessing cost after COVID-19
The COVID-19 crisis has altered the landscape for many. Some have already acted to reduce staff numbers and consolidate operations as an initial response to falling revenues. Structural change and a lower cost base may be required to adapt for the longer term driven by:
- Altered demand volumes, market location and mix of products and services as markets and the customer base evolves
- New regimes to protect health and wellbeing that change how people can work
- The increasing de-globalisation trend, prompting a re-think on the resilience of supply chains and moves to localise
The scenarios and options for each business will be different and the ‘best fit’ answer will not necessarily be obvious.
Considering the case for structural change
Supply-side capacity
- What capacity is needed now and for the medium term? Can excess capacity be re-purposed to meet expected new demand or is consolidation possible?
- Restructuring the footprint is an opportunity to deliver a step change in the cost base and renewed focal points for future investments
Network view
- How fit for purpose are existing facilities now? Can a more cost-effective and resilient model be found by looking at the network as a whole?
- Potential changes to both demand and supply-side environments will impact the economics of the current model and an holistic view is needed
Supply chain
- Will customers demand more localised sourcing to reduce interruption risk in their business-critical supply chains? Is a pre-emptive move to adapt the footprint more attractive than a reactive one?
- Sourcing and certifying new suppliers may be a critical dependency for re-locating production. It is also an opportunity to re-think make-buy strategies, secure new capabilities, strengthen key supplier relationships and unlock cost savings
Overhead right size
- What opportunities from changed working practices should now be evolved to deliver a lower overhead cost model?
- Remote working, greater comfort with and reliance on technology, and demonstrated operation with reduced indirect staffing levels creates new baselines for the operating model
Digital evolution
- What opportunities are created through a reshaping of the footprint to accelerate adoption of digital technologies?
- Relocation of capabilities to be better aligned with future demand will require assessment of products, processes, assets, resources and technology infrastructure. Introduction of technology to deliver cost and service advantage may be achieved in a more concentrated way, more quickly and with greater impact as part of a footprint reshape than through retrofit in a sub-optimal model
Affordability
- How will transition be funded and what prioritisation is required? A balanced-risk business case and plan are needed
- Parallel effort to drive out non-value-add activity, reduce working capital and target efficiencies in the current model will create additional headroom to manoeuvre
Having dealt with the immediate threat from COVID-19, executives, stakeholders and shareholders are now turning their attention to what comes next.
Businesses that are proactively considering the options now will be better placed to make the right moves to sustain and grow.
How we can help
We have broad experience of working with industrial clients to deliver higher levels of profitability and resilience by optimising the cost base, with managed risk and without compromising business value-add service delivery.
Our bespoke Assessment Model is a tried and tested approach balancing commercial, financial and operational considerations. We can rapidly examine the possibilities, frame the options and quantify the associated benefits and risks to underpin confident decision-making.
We bring a business-led focus, an insight-driven approach and a pragmatic attitude to help our clients make informed decisions. And where needed we assist in delivering the business case.
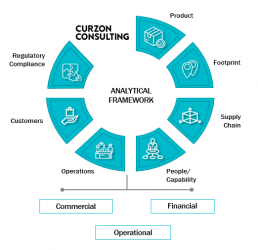
Contact us to explore how to deliver a more resilient and cost optimised business in a post-COVID environment.
Want to find out how our Industry & Energy Services consulting team can help?
Infrastructure after Covid-19 – when the mould is broken where do you want to be?
Competition or collaboration? Navigating change in infrastructure after Covid-19
The Covid-19 pandemic has brought about rapid unprecedented change. Companies have responded to imposed restrictions, people have adapted to new ways of working, and the impact on the economy, employment and productivity has been immense.
Businesses face an ever-shifting timescale for recovery but uncertainty on how they need to adapt in the short, medium and longer term.
A commitment to investment in infrastructure
With uncertainty over the shape of economic recovery, the UK government is under increasing pressure to provide answers. The current political agenda is balancing the risk of further outbreaks against the need to kick-start the economy and get people back to work. Infrastructure is a key part of this recovery plan.
As such, we are seeing a range of statements, commitments and emerging policies that::
- Commit to accelerated investment in infrastructure
- Criticise past failings in the delivery of major programmes which have taken too long and cost too much
- Question how other countries can do it so much better than us
- Recognise that we have developed a huge burden of bureaucratic processes
- Challenge the slow adoption of new technologies and innovation
- Reinforce previous goals on climate change and the environment
What does this mean for core infrastructure and regulated industries?
The services and facilities provided by infrastructure and regulated industries are essential to the future growth of the economy. The challenge is how to fairly manage the cost of recovery, which will ultimately be passed onto the consumer. This creates further pressure on the whole system including clients and service providers. Some key questions and considerations include:
For Clients (or sponsors)
- With greater pressure on household budgets, customer expectations on service and value will increase
- Customers will be less tolerant of failure and companies will be under greater scrutiny
- Social and environmental conscience is increasing
- As a result of COVID-19 there will be sustained change in the way people work. But is the full impact fully understood?
- Clients or sponsors will be under increased pressure from the regulators to deliver more for less
- Continuing to stretch existing resources and deliver incremental change will not be enough
- Companies will be driven to develop different and more efficient operating models
For Service Providers
- No longer contractors or consultants but “Service Providers”
- Has traditional contracting had its day and does it really deliver what clients and customers are ultimately looking for?
- Service Providers will be under the greatest pressure to address the higher-level challenges through creating new ways of working or new service offerings
- “Necessity is the mother of invention” – the time of greatest need will drive the greatest change and the more agile companies will be those that win
- Traditional contracts delivered in a traditional way will become an increasing “race to the bottom” based on price with associated increase in failure
Innovation and technology inevitably has a major part to play in addressing the above.
What part should Innovation and Technology play?
Regulated industries are notoriously slow adopters. If this is to change, it is essential to understand the reasons why and break these paradigms.
- Risk of failure is too high either in terms of impact on customers or regulatory action
- Procurement processes are cumbersome and often preclude SMEs/Start-ups
- In reality, Intellectual Property has a very short shelf-life, products are quickly copied
- There is more to be gained from running faster and letting others follow compared to standing still and protecting what you have got
With many organisations facing the same challenges, is there something to be learned from collaboration?
Competition or Collaboration?
Regulation has often been based on the premise of driving or simulating competition. So, what delivers the greatest benefit – organisations collaborating or competing? Many “alliance” delivery models are based on the benefits of collaboration which raises a number of questions:
- Regulated utilities by their nature are often monopolies so why isn’t there far greater collaboration and sharing of ideas?
- Technology/Innovation start-ups often have to prove their concepts several times over to separate clients passing through individual tortuous procurement routes. As a result many collapse before they start. As a wider industry why do separate companies re-invent the same wheel
- Contractors/Service Providers provide similar services to different clients and sectors in the same geographic area. Is there more to be gained from a common approach across sectors?
- If the same Service Provider is providing a service across multiple clients and sectors who is the regulator actually regulating – the Client or The Service Provider?
- If the end service across sectors is a similar service why should there be different regulatory models and different regulatory measures or even different regulators?
Acceleration, adaption and adoption
The COVID-19 pandemic has had an undeniable impact on organisations. Businesses have been forced to adopt a more radical and agile approach in how they adapt to change.
This unprecedented challenge has also created opportunities. Many businesses have failed but some have flourished. In the main, these organisations have embraced a culture of learning from others. They have collaborated and openly shared resources. They have undertaken the accelerated development of complex solutions and executed them with simplicity.
Going forward, significant commitments have been made, expectations are high and pressure on delivery will increase. The challenges will necessitate change and those that move fastest stand to gain the most.
The authors
Get in touch
We help infrastructure organisations to meet challenging targets through strategy, operating model design and transformation.
Contact us to discuss how we can help your organisation.
Want to find out more or meet one of our Infrastructure team? Contact us by email, phone or our web form.
Digital productivity management in infrastructure
The full package: digitising productivity management in infrastructure delivery
Infrastructure owners and construction companies are selecting or developing, and then seeking accelerated implementation and scaling of, their preferred digital productivity management tool(s).
In consideration of the current economic climate, the critical role that Infrastructure investment is set to play in boosting growth has been amplified.
In light of these two factors, it does not feel as though there could be a better time to suggest that if we are going to do the whole ‘digital productivity thing’ in infrastructure and construction… we should do it properly. So, what does ‘doing it properly’ mean? It means that it is time to assess the full spectrum of construction-site productivity management capability areas that can be enhanced through the new or improved application of digital tools. We need the full package.
Unlocking greater efficiencies through digital
Digital enablement has revolutionised productivity and the definition of efficiency norms in other industries. Most notably in Manufacturing industries such as Fast-moving consumer goods (FMCG) where market leaders such as Unilever have reduced material factory waste by more than 40% by digitally enabling end-to-end quality management. (Source: World Economic Forum, How manufacturing can thrive in a digital world and lead a sustainable revolution, January 2020)
Similarly, by 2025 the digital enablement of Logistics has the potential to reduce global carbon emissions by 11%. (Source: World Economic Forum, Digital Transformation of Industries Demystifying Digital and Securing $100 Trillion for Society and Industry by 2025, January 2016) A powerful endorsement of advanced productivity management tools.
The Agriculture industry presents further evidence. Here, as an example, data gathering and historical analysis data-driven decision-making tools are having a transformative impact on crop productivity.
Productivity management in infrastructure however is often driven by manual cost and performance benchmarking processes. Some efficiency gains have been achieved through the successful adoption of Lean methodologies. But the meaningful use of digital tools that enable higher productivity rates will be key to unlocking much greater efficiencies in the construction phases of infrastructure programmes.
There is an entire spectrum of construction site productivity management capability areas that can be enhanced through the application of digital tools. These can be broadly placed into three categories:
- Planning and Collaboration: Ensuring the feasibility of planned activities and improving communications between the site and site-office
- Data gathering: Gathering data on the work accomplished on-site to feed performance/progress metrics
- Data-driven analytics: Collecting historical productivity data on-site to feed data-driven decision making
In pursuit of significant improvement
Organisations tend to focus on the independent application of a discrete digital tool to enable productivity. Most often this means dedicating themselves to a data gathering tool for the purpose of productivity tracking. However, in the pursuit of significant efficiencies it is not sufficient to introduce digitally enabled capability to just one area of the productivity management spectrum. For infrastructure delivery, at the construction site level, a suite of digital tools covering the full range of capabilities (outlined at a high level by the three categories above) is required. Many of the more recently developed tools incorporate data as a service (DaaS) offerings but there is the opportunity to go further. Attributes for productivity information gathered, processed and analysed should adhere to the standards set by data and information frameworks being built by infrastructure owners.
For data generated by any suite of tools, there is the opportunity to actively inform cost and performance benchmarks and subsequently productivity norms for the delivery of work. This applies within the integrated environment for information that programmes, alliances or organisation level data frameworks house.
So how to decide on which digital productivity management tools to work with?
Whether through in-house development or accessing solutions already in play, several factors should be considered, including but certainly not limited to:
- Ease of implementation
- Supply chain buy-in
- Scalability across multiple construction disciplines
Prioritisation frameworks can be designed and applied to rapidly assess an entire landscape of digital productivity management solutions, thoroughly reviewing each through the lenses of standard attributes.
Digital productivity done properly
Individual tools applied in isolation in areas such as productivity tracking can offer benefits. But there is an entire spectrum of on-site productivity management capability that can be enhanced through the application of digital tools. These benefits can be amplified through alignment with the principles for data defined by information frameworks being developed by infrastructure owners. Other industries are demonstrating the scale of productivity benefits available through digital enablement. These are most notable where a complete end-to-end process approach is adopted.
So, if we are going to do the whole ‘digital productivity thing’ in infrastructure and construction… we should do it properly.
The authors
How we can help: Rapid Digital Portfolio Prioritisation
Siloed innovation, functional misalignment and data ‘doing its own thing’ are just a few challenging features of the current congested-frontier of digital transformation.
Applying our bespoke prioritisation framework(s), Curzon Consulting takes 4-6 weeks to rapidly assess an organisation’s entire landscape of digital solutions and initiatives. We thoroughly review each through the lenses of attributes that are orientated around features such as financial benefit, scalability and interoperability.
Get in touch to find out how we can help or arrange a free virtual meeting with award-winning Principal consultant, Edem Eno-Amooquaye.
Want to find out more or meet one of our Infrastructure team? Contact us by email, phone or our web form.
The accelerated adoption of drones in healthcare
We explore how the 2020 coronavirus crisis has accelerated the use of drones in the delivery of healthcare.

Drones in Healthcare
The commercial use of drones has steadily been gaining traction over the last decade.
The global market for medical drones was valued at USD $88.2 million in 2018. It is expected to witness 24.7% CAGR from 2019 to 2025. The UK market is anticipated to see even higher than 25% CAGR from 2019 to 2025. The global circumstances resulting from the coronavirus pandemic are likely to increase demand for unmanned aerial vehicles (UAVs) and drive the value of the drone market up even higher than forecast.
Drones have the potential to transform the delivery of healthcare. They have a large spectrum of medical uses that could be particularly valuable during this pandemic:
- Search and Rescue: searching vast areas for people in need of rescue/help in any environment
- Transport/Delivery: rapid delivery of medical supplies to rural areas between hospitals/labs or directly to the person in need
- Medical Care: remote delivery of medical advice/care
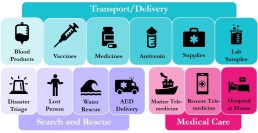
Despite wide potential applications in healthcare, the use of drones in practice has been fairly limited. Safety and security concerns have led to tight regulations on airspace. This makes it difficult to phase in drones for practical (rather than recreational) use. Drones have a bad reputation due to their potential abuse in breaching privacy, violating human rights and irresponsible use by hobbyists, particularly at airports. Consequently, only a small proportion of the potentially vast benefits offered by drones in healthcare have been realised.

COVID-19 impact on drones in healthcare
The coronavirus crisis has acted as a catalyst for the adoption and acceptance of drones in healthcare. There are two main reasons for this:
- The need to deliver medical care/supplies quickly is more urgent
- Social distancing and quarantine measures have made remotely operated systems particularly valuable
As a result of coronavirus, how has drone use changed or adoption accelerated? We’ve included some examples below.
Dutch company Avy manufactures wing drones for use in urban healthcare logistics, rural delivery of supplies, and first response emergency services. Avy responded to the pandemic by exploring the use of wing drones to transport COVID-19 samples from small municipalities to labs in larger cities. This would help contain the virus and minimise risk of the virus spreading.
We spoke to Patrique Zaman, Founder of Avy, about the healthcare challenges that Avy is trying to overcome.
This is an example of a drone company, Manna Aero, that changed their focus from food delivery to medicine delivery during the pandemic.
The Irish start-up launched their drone delivery service earlier this year, with the aim of moving road-based food delivery into the skies. Manna Aero’s trial delivery of takeaways to college students in mid-March had to be halted due to the coronavirus lockdown, but this did not deter them from switching focus to help in the crisis. The company has instead been working with the Irish Health Service Executive to deliver medicines and other essential supplies such as break and milk to vulnerable people in the rural town of Moneygall. Local GPs write prescriptions after a video consultation, which the drones deliver directly to homes. This represents a first in Ireland. Manna Aero is equipped to handle up to 100 deliveries a day, and hopes to bring trials to the UK soon.
The UK’s lockdown in 2020 triggered the government to grant permission for a UAV to deliver medical supplies across the Solent to a hospital on the Isle of Wight. This is part of a UK government project to develop a system allowing manned and unmanned aircraft to operate in the same airspace.
The UAV, developed by the University of Southampton and funded by the start-up Windracers, was given permission to fly as part of the British government’s Covid-19 response. It has a range of 1,000km and can carry up to 100kg.
Compared to the more traditional ferry, this novel approach allows faster, more frequent, and more reliable delivery of medical supplies.
The Covid-19 response has triggered a partnership between the drone delivery provider Skyports and Thales to trial the delivery of medical supplies.
The two-week pilot is backed by NHS Highland, and Argyll and Bute Council, with drones supplied by unmanned aircraft-maker Wingcopter. The delivery service will be based in Oban. It aims to ensure that isolated communities on the Isle of Mull (16km away) have access to COVID-19 tests and sufficient personal protective equipment (PPE).
This trial is a crucial milestone for unmanned aviation in the UK. It was granted as an exception to current rules by the Civil Aviation Authority.
Zipline is a US drone company that delivers supplies to rural communities in Rwanda and Ghana. In order to support the Covid-19 response in Africa, Zipline changed its focus to using drones to provide clinics with PPE and coronavirus test samples. The lightweight drones deliver to clinics up to 85km away. There are plans to use the drones to deliver supplies directly to the elderly and vulnerable who need to self-isolate.
Zipline CEO Keller Rinaudo thinks that drone deliveries could play a vital role both during the current crisis and in the coming months and years.
The Chinese government has been proactive in piloting ways to incorporate drones into their response to the coronavirus.
Drones originally designed to spray pesticides have been adapted to spray disinfecting chemicals in public spaces. Testing the use of drones to deliver of medical samples began in February, with over 20 flights per day at peak operation in Zhejiang Province. Consumer delivery of essential items has also been trialled, with e-commerce company JD developing a drone team to deliver to Anxin’s semi-isolated islands.

Future outlook
The unprecedented circumstances brought about by Covid-19 have kick-started the use of drones in new and exciting ways, but we are only scratching the surface of their full potential.
To progress, we need to learn from this pandemic and make changes that will ultimately lead to a better healthcare experience. Rather than relying on experimentation, we should pre-plan how drones can be used during disease outbreaks and make appropriate investments. Drones need to be integrated into planned health responses. In addition, coordination between the public and private sector will be crucial to overcome regulation by civil aviation authorities.
It is obvious that drones have a big role to play in the delivery of healthcare. The route to unlocking their true potential will offer exciting and rewarding opportunities in the future.
How Curzon can help
Curzon Consulting help with strategy and digital transformation. We have experience working in collaboration with companies to embed technology into their organisation. Curzon can:
- Conduct feasibility studies
- Build a business case and commercial offering
- Design the most appropriate operating model and integration plan
- Conduct a technical requirement assessment
Get in touch to find out how we can help or arrange a free virtual meeting with our Healthcare partner, Chetan Trivedi.
The authors
We can help you to improve patient outcomes with digital strategy, transformation and patient experience.





























